Sachar Dental NYC
For SAME day / emergency appointments
Call (212) 752-1163
All the below content has been written by NYC Dentist, Dr. Sandip Sachar.
Dentist NYC - Periodontal Surgery
On this page: (Click topic below)
What is pocket reduction surgery?
Why would I need pocket reduction surgery?
What are the goals of pocket reduction surgery?
How is pocket reduction surgery done?
Dental implants
What are dental implants?
Why would I need dental implants?
How is a dental implant placed into my mouth?
What is soft tissue grafting?
What causes gum recession?
Why would I need soft tissue grafting?
What are the benefits of soft tissue grafting?
How is soft tissue grafting done?
What is ridge modification surgery?
What is crown lengthening surgery?
Why would I need a crown lengthening surgery?
How is crown lengthening surgery done?
What is bone grafting?
Why would I need bone grafting?
How is bone grafting done?
What is a sinus lift?
What are the different types of periodontal surgery?
- Pocket reduction surgery
- Dental implants
- Soft tissue grafting
- Gum grafting
- Gum recession surgery
- Ridge modification
- Crown lengthening
- Bone grafting
- Sinus lift
- Sinus augmentation
What is pocket reduction surgery?
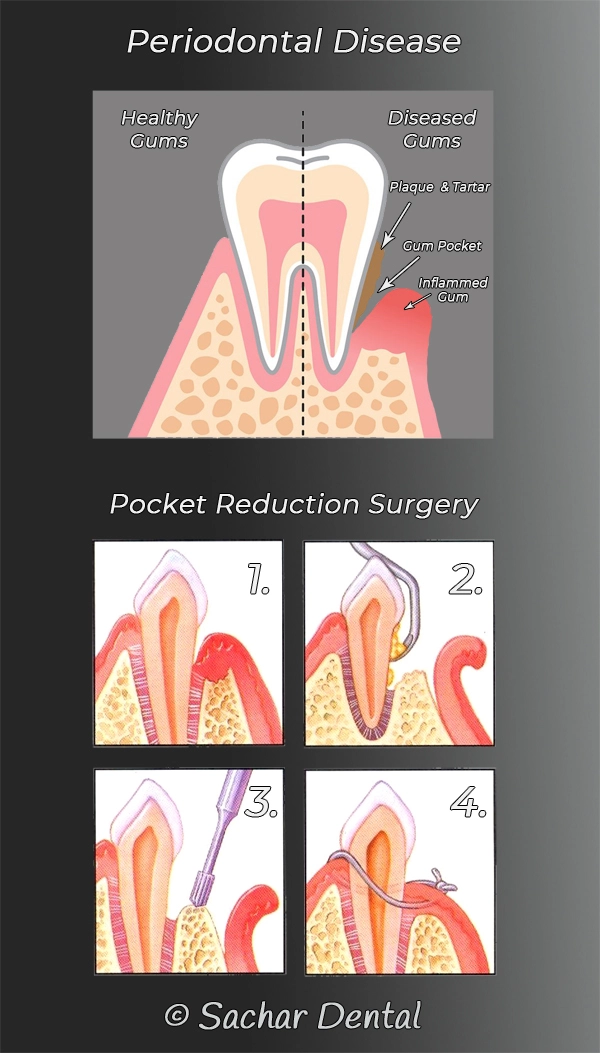
Pocket reduction surgery has also been called gingivectomy, osseous surgery, and flap surgery. All of these terms describe periodontal surgery with the goal of gaining access to the roots of the teeth, under the gums, in order to remove bacteria, plaque and tartar.
Periodontal disease occurs when the gum pockets are greater than 3 mm and contain plaque, tartar and bacteria. The gum pockets are the spaces between the tooth roots and the gums. In the early stages, a deep dental cleaning may be able to remove bacteria from the gum pockets and is the first step in periodontal disease treatment. When a deep cleaning fails to remove all bacteria and prevent deep gum pockets, periodontal pocket reduction surgery is indicated.
Left untreated, bacteria in the gum pockets can eventually lead to loss of bone, loose teeth or tooth loss. Pocket reduction surgery may be able to prevent these sequelae from happening.
Why would I need pocket reduction surgery?
Patients that have undergone a deep cleaning for periodontal disease, and that has failed to remove all bacteria and/or reduce the deep gum pockets, will then be candidates for pocket reduction surgery. Patients that have also been diagnosed with moderate to advanced periodontal disease and have had bone loss, are also candidates for pocket reduction surgery. Pocket reduction surgery allows our periodontist to gain access to the deep gum pockets and remove plaque, tartar and bacteria.
What are the goals of pocket reduction surgery?
Reducing bacterial spread – pocket reduction surgery allows our periodontist to access the deep gum pockets in order to remove bacteria and prevent its spread. Left untreated, bacteria may spread through the bloodstream and end up infecting other bodily organs. Bacteria can also cause the erosion and loss of bone leading to loose teeth, or teeth that fall out.
Halting bone loss – left untreated, bacteria in the gum pockets can slowly destroy the jaw bone where the teeth attach. Over time, this can lead to loose teeth, or teeth that fall out. It may also necessitate us to perform a tooth extraction.
Facilitate home care – when deep gum pockets are present, it makes it difficult or impossible for patients to remove plaque and bacteria with regular flossing and brushing. This can lead to the progression of periodontal disease and eventually erosion of the jaw bone, and tooth loss. After pocket reduction surgery, home care with brushing and flossing is much easier for patients to remove bacteria and plaque.
Enhancing the smile – with more advanced periodontal disease, the gums do not appear normal. Typical symptoms of periodontal disease that are cosmetic include discoloration of the gums, rotting teeth, and indentations in the jaw bone. Pocket reduction surgery may be able to stop the progression of periodontal disease and improve the aesthetics of the smile. Often, we perform bone grafts along with pocket reduction surgery in order to restore the contour of the jaw bone, making it look more normal.
How is pocket reduction surgery done?
The first step in pocket reduction surgery is making the diagnosis of the necessity for this procedure. Our periodontal specialist will first do a clinical examination and perform x-rays. He will assess the condition of the gums, bone and teeth. Patients who have periodontal disease and deep gum pockets often will first undergo a deep dental cleaning to see if that is enough to treat the periodontal disease. For patients that fail deep cleaning in order to stop the progression of their gum disease, they will be candidates for pocket reduction surgery. Additionally, patients that exhibit moderate to severe periodontal disease and bone loss, are also candidates for pocket reduction surgery.
Pocket reduction surgery is done under local anesthesia in order to prevent pain and discomfort during the procedure. The periodontal specialist will pull back the gums from their attachment to the teeth and access the deep gum pockets. This allows access to the roots of the teeth and under the gums. We will then inspect and remove any plaque, tartar and bacteria that are found in the deep pockets. Root planing is a process of smoothing the surface of the root such that the gums can reattach and bacteria cannot attach. In some cases, we may administer injection of antibiotics to prevent recurrence of bacterial infection. And finally, the gums are then sutured in place.
Dental implants
Dental implants are permanent solution for missing teeth. They are able to function normally and cosmetically look normal as well. The term ‘dental implant’ is often used by the layperson to describe a single tooth dental implant that consists of three pieces, an implant, an abutment and a crown. The actual dental implant is the part that is inserted into the bone. The part that replaces the tooth that is visible is called the crown. The crown attaches to the implant using an abutment. Besides restoring the appearance of your smile, they can also restore the function after a tooth that has been removed.
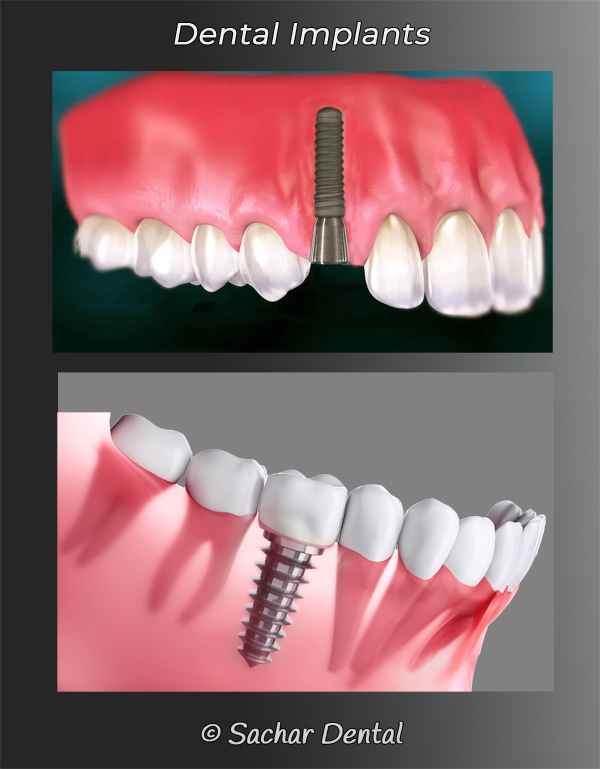
What are dental implants?
When discussing the terminology related to dental implants, there may be some discrepancy or vagueness. In medical terminology, the dental implant is only the part that is placed into the bone to replace the root, and does not include the crown (artificial tooth) or the abutment.
Dental implants are used to replace missing teeth. A dental implant is a metallic device that is screwed into the jaw bone that acts as an anchor for a crown to replace a tooth, or an anchor for a bridge or denture to replace multiple teeth. Multiple teeth can also be replaced with multiple individual implants.
Why would I need dental implants?
There are many reasons why one may lose a tooth. Whatever the cause for the loss of a tooth, a dental implant is in excellent option to replace the tooth in order to restore the function of chewing, speaking and aesthetics. Tooth loss may occur as a result of:
- Damaged teeth due to tooth decay
- Gum disease, periodontal disease
- Fractured teeth
- Trauma
- Infection
How is a dental implant placed into my mouth?
The first step before inserting a dental implant is to perform a tooth extraction to remove the diseased or traumatic tooth. We will also perform a clinical examination and x-rays to assess the bone. The bone needs to be strong enough to support the dental implant going forward. If we determine that the bone is not strong enough to support the dental implant, we will perform an additional procedure such as a sinus lift or a bone graft. On the same visit sometimes, or subsequent visit sometimes, the implant is then placed into the bone. At Sachar Dental NYC, our implant specialist will decide the timeframe of your treatment. Some patients may have an extraction, bone graft and insertion of a dental implant on the same visit, or over multiple visits.
The process of getting a dental implant requires multiple visits. After the implant is placed into the bone, it is allowed to heal before the next visit. Once we determine that the bone is healed, the implant is then ready to receive an artificial tooth, or multiple teeth attached to it. We will take x-rays to evaluate the bone healing. Once we are sure that the bone is healed, we will take a mold that is used to make the crown, bridge or denture. We will send this mold to our dental laboratory who will fabricate your appliance.
During the course of your implant procedure, for cosmetic reasons, we will provide you with a temporary crown or a flipper to fill the space where the tooth was removed.
Once we receive your permanent teeth replacements from our laboratory, we will have you come in to attach them to the implants. We will then give you detailed instructions on how to care for your new teeth.
What is soft tissue grafting?
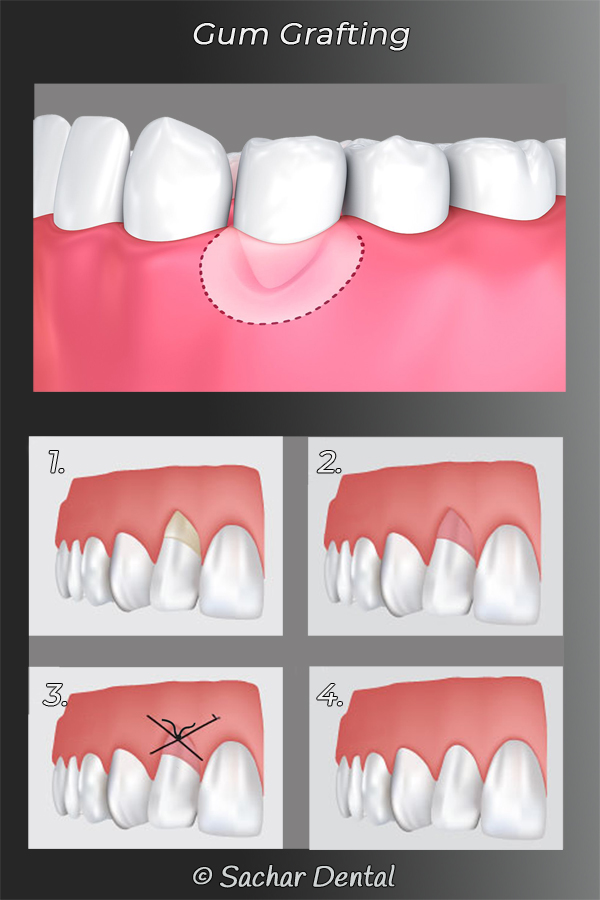
Soft tissue grafting is also called gum grafting and gum recession surgery. Gum grafting is an in-office dental surgical procedure that is used to move the gums in order to cover the exposed tooth root. It is both cosmetic and functional. Exposed tooth roots are usually the result of periodontal disease. Other possible causes include aging, overaggressive brushing, clenching and grinding and other trauma.
Gum recession
Gum recession is also called “gingival recession”. This refers to the progressive loss of gum tissue and eventually can lead to the exposure of the tooth root.
What causes gum recession?
Often, gum recession is diagnosed during your routine dental checkups every 6 months. It is best to catch it early before it is more advanced and noticeable. Gum recession can be caused by multiple factors including:
Overaggressive brushing that can lead to erosion of the gums. This happens when one brushes too hard or uses hard bristle toothbrushes. This can also lead to inflammation of the gums and eventually also erosion of the tooth enamel.
Poor oral hygiene can also lead to gum recession. The build-up of bacteria and plaque on the teeth and under the gums can lead to periodontal disease. This can eventually erode the underlying jaw bone which can lead to teeth that become loose and eventually fall out. It is caused by bacteria and plaque that builds up in the gum pockets. Deep gum pockets harbor bacteria that cannot be removed with flossing and brushing alone. Left untreated, bacteria can eventually erode the jawbone and cause loose teeth or teeth that fall out.
Clenching and grinding of the teeth can also lead to gum recession. This aligned teeth also can lead to gum recession. In both of these cases abnormal forces on the teeth can lead to excessive load on the teeth which causes gum recession.
Why would I need soft tissue grafting?
Anyone that has experienced gum recession with exposed tooth roots may be a candidate for soft tissue grafting or gum grafting. Gum grafting can be both cosmetic as well as functional to make the appearance of the teeth improved and prevent symptoms such as sensitive or painful teeth.
What are the benefits of soft tissue grafting?
Increased comfort – having expose tooth roots can cause pain, discomfort and sensitivity. This can occur with eating foods that are hot or cold or just chewing. Gum grafting is able to cover the exposed roots which helps to reduce discomfort, sensitivity and pain.
Aesthetic improvement - a gum grafting surgery can cover the exposed roots of the teeth make them look more normal and patients look younger. Having gum recession often leads to a “toothy smile” where the teeth look much longer. Gum recession can also cause to the teeth to look uneven in size. Gum grafting can make the smile look more symmetrical, and more natural.
Improved gum health – after periodontal disease treatment, gum grafting can assist in preventing its recurrence. It can help to stop the progression of bone loss and prevent problems associated with the exposed tooth roots. It is able to help protect the roots of the teeth from further complications.
How is soft tissue grafting done?
Prior to performing a gum graft, our dentists will identify the cause of your gum recession. They will then address these factors prior to performing a soft tissue graft or gum. For example, when periodontal disease is present, the periodontal disease has to be treated first in order to remove the bacteria from the gum pockets. Then, a gum graft may be utilized to cover the exposed tooth roots.
Gum grafting is done under local anesthesia to ensure its comfort. Our periodontal specialist will separate the gums from their attachments to the jaw bone and the teeth. He will then advance the tissues to cover the roots of the teeth and suture them in place.
What is ridge modification surgery?
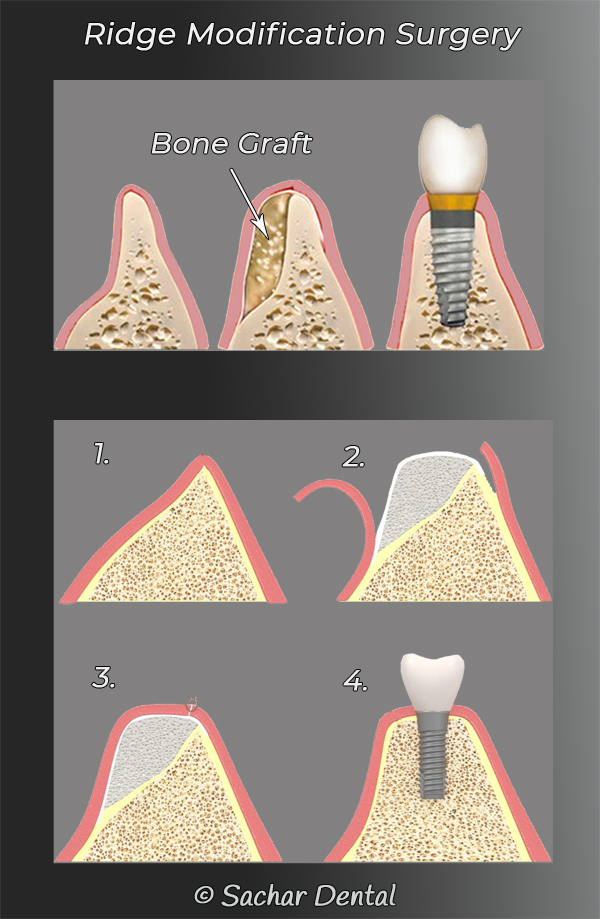
Ridge modification surgery is utilized to correct for loss of bone in the jaw bone. It may be done in order to provide enough bone to support a dental implant, or be done for cosmetic reasons to improve the aesthetics of the jawbone that shows areas of deficit. For ridge modification surgery, local anesthesia is used. Our periodontal specialist will lift the area of the gum that is attached to the bone where a deficit is identified. The bony defect will be filled with bone grafting material. The gums are then sutured in place. Ridge modification surgery improves the cosmetic appearance as well as the function of the jaw bone. It also allows for future implantation of the dental implants into the bone that previously would not be strong enough to support it.
What is crown lengthening surgery?
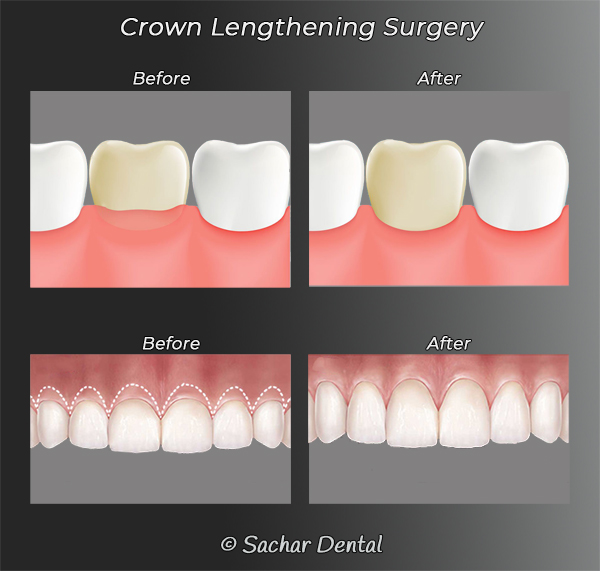
Crown lengthening surgery is performed when there is not enough of the natural tooth exposed in order to anchor a crown. In this case, our periodontal specialist will remove some of the attachment of the gums and the attachment of the bone around the root of the tooth. This allows us to expose more of the tooth. We will then have enough surface area to permanently bond a crown to the tooth.
Why would I need a crown lengthening surgery?
When patients need a crown, and there is not enough of the remaining tooth exposed in order to bond the crown to the tooth, they may need a crown lengthening procedure. This may occur from having damaged teeth due to periodontal disease or trauma. In these cases, the tooth may have broken at, or under, the gum line. A crown lengthening procedure exposes more of the tooth in order to allow us to permanently bond a crown to the tooth.
How is crown lengthening surgery done?
Crown lengthening surgery is an in-office dental procedure that is done under local anesthesia. Once local anesthesia is achieved, our periodontal specialist will gently separate the gums from their attachments to the teeth and bone. For some patients, this is enough to expose the tooth in order to bond the crown. In other patients, it may be necessary to remove a small amount of bone from around the tooth root.
We will then allow 2-4 weeks for the healing process to complete. At this stage, we will take a mold of the tooth in order to send it to our dental laboratory to make the crown. When we receive the crown, we will then bond it permanently onto the tooth.
What is bone grafting?
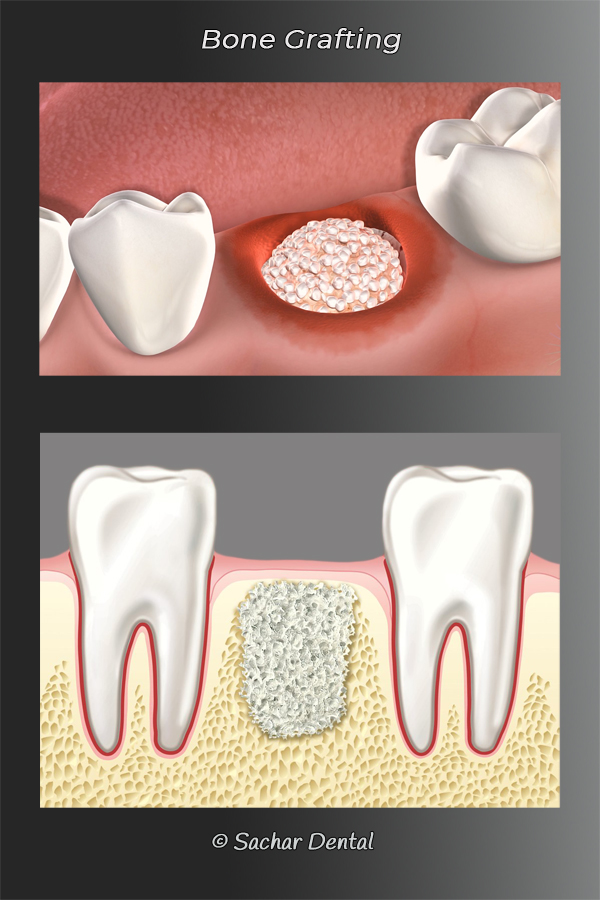
The most common cause of bone loss in the jaw bone is periodontal disease. Bone grafting procedures are used to replace some of the lost bone. The purpose of replacing the lost bone may be cosmetic or to make the bone stronger such that it can support a dental implant.
Why would I need bone grafting?
Some patients will require a bone graft in order to make the bone stronger in order to support a dental implant. Our periodontal specialist will identify when this is necessary prior to placing dental implants. It is important to have strong bone under a dental implant to ensure that it does not fail.
Similarly, in the upper jaw, a sinus lift may be necessary which also entails a bone graft. In this case, the bone of the upper jaw between the mouth and the sinuses may become too small to allow for the implantation of a dental implant. Sinus lift surgery enables us to place a dental implant by making the bone thicker and the sinus higher.
Loss of bone in the jawbone can lead to some unsightly ridges where the bone has been lost. Ridge augmentation uses bone graft to fill in these deficits and make the jawbone look more uniform and normal in shape and size.
How is bone grafting done?
Bone grafting is done under local anesthesia. The site where the bone graft is necessary is identified. This area is then prepared to receive the bone graft by filing a small amount of bone to create an area for the bone graft to attached to. The proper amount of bone grafting material is then placed into the deficit. A membrane is then inserted over the bone graft in order to hold it in place and help with the healing process. The gums are then sutured in place. The soft tissue of the gums will cover the bone graft and the membrane. Over time, the body will incorporate natural bone into, and replacing the bone graft in order to create bone that is similar strength to the natural bone.
What is a sinus lift?
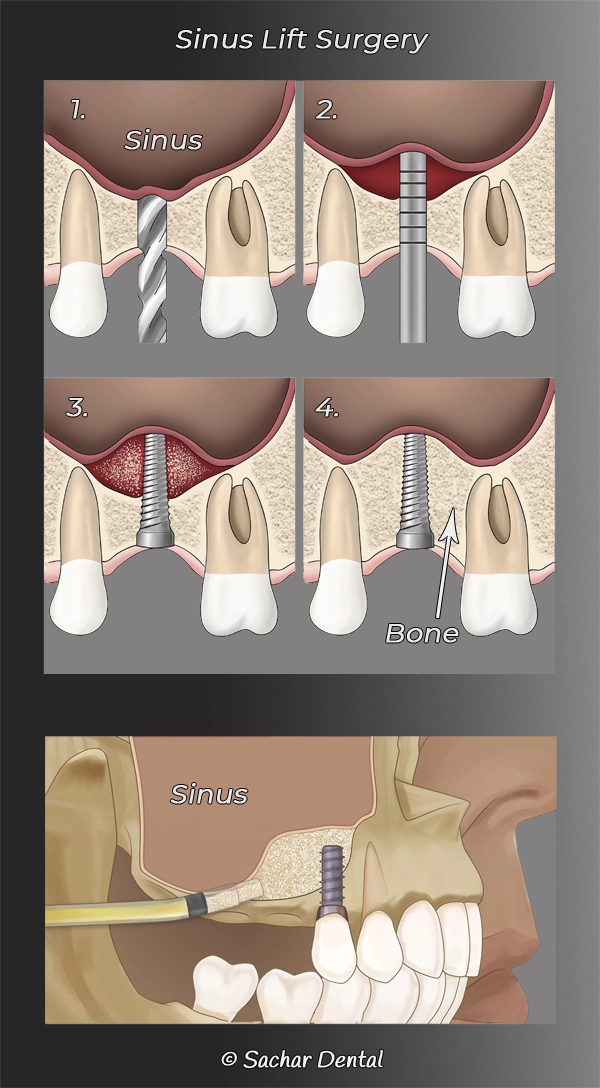
In the upper jaw, directly on top of the jawbone are the sinuses. When there is erosion of bone, the bone between the teeth and the sinuses may become very thin. When this happens, it is not possible to place implants without invading the sinus. The sinus lift procedure enables our periodontal specialist to use a bone graft to make the bone thicker, as well as lift the sinus up such that the implant will not penetrated into it.


